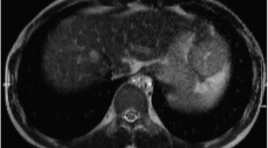
NGHIÊN CỨU KẾT QUẢ BƯỚC ĐẦU ĐIỀU TRỊ UNG THƯ BIỂU MÔ TẾ BÀO GAN BẰNG PHƯƠNG PHÁP ĐỐT SÓNG CAO TẦN TRONG MỔ
14/10/2023 12:09:21 | 0 binh luận
SUMMARY Intraoperative radiofrequency ablation is a new approach for the radical treatment of patients with multifocal hepatocellular carcinoma in different lobes. Originally, patients no longer indicated for radical treatment were now surgically removing the tumor in one lobe and radiofrequency ablation of other tumors in the surgery period time. Objectives and subjects: A retrospective and prospective study conducted between 2020 and 2022, 09 patients with HCC with at least 2 tumors in different lobes underwent intraoperative radiofrequency ablation (IORFA) and followed-up for 3 months at Bach Mai Hospital. Results: All 09 patients with 28 tumors, the number tumors from 02 to 06, each patient underwent surgery to remove 01 large tumor and radiofrequency ablation in surgery for other tumors. All patients responded completely according to mRECIST criteria, no local recurrence, relapsed or died within the first 3 months. Conclusion: Intraoperative radiofrequency ablation is a new effective method approach, help to expand the indications for radical treatment for patients with multifocal hepatocellular carcinoma. Keywords: Intraoperative radiofrequency ablation, hepatocellular carcinoma. *

Case lâm sàng: nhân một trường hợp chụp và can thiệp bạch mạch đái dưỡng chấp tại trung tâm điện quang bệnh viện Bạch Mai
20/04/2021 13:30:28 | 0 binh luận
Đang cập nhật
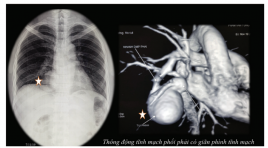
Dị dạng rò động tĩnh mạch phổi lưu lượng lớn: ca bệnh hiểm được chẩn đoán và điều trị can thiệp nội mạch
02/06/2020 11:07:52 | 0 binh luận
Pulmonary arteriovenous fistula case report: diagnosis and endovascular treatment SUMMARY Pulmonary arteriovenous malformations (PAVM) are rare pulmonary vascular anomalies. Although most patients are asymptomatic, PAVMs can cause dyspnoea from right-to-left shunt. Because of paradoxical emboli, various central nervous system complications have been described including stroke and brain abscess. There is a strong association between PAVM and hereditary haemorrhagic telangiectasia. Chest radiography and contrast enhanced computed tomography are essential initial diagnostic tools but pulmonary angiography is the gold standard. Contrast echocardiography is useful for diagnosis and monitoring after treatment. Most patients should be treated. Therapeutic options include angiographic embolisation with metal coil or balloon occlusion and surgical excision. We present a clinical case in a 33-year-old male patient, diagnosed with a large, single PAVM in the right lower lung with X-ray and CT scan. Patients treated with pulmonary angiography embolisation with 2 metal coil and plug14, rechecked after 6 months by magnetic resonance, computerized tomography and pulmonary angiography, complete loss of shunt stream. Clinically improved, blood gas test before intervention: pO2 64.7mmHg and SatO2 89.9% and 6 months after intervention: pO2 91.3mmHg and SatO2 96.2% . Key word: arteriovenous fistula, embolization, pulmonary vascular malformation
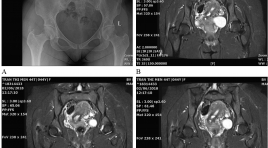
Nhân một vài trường hợp điều trị viêm gân vôi hóa bằng chọc hút vôi dưới hướng dẫn siêu âm
05/12/2019 10:11:45 | 1 binh luận
Report of several cases of treatment of calcific tendonitis by aspiration under ultrasound guidance SUMMARY Calcific tendonitis is a common disease caused by the deposition of canxi hydroxyapatite crystals in the tendons. The disease can occur in all tendons in the body and also in the ligaments, but the most common sites are the tendons of rotator cuffs , tendons around great trochanter, tendons around elbow joints, wrists... Normally, there is no pain. However, as calcification resorption occurs because the body releases enzymes that resolve calcification, patients develop severe and persistent pain. In terms of diagnosis, clinical symptoms are quite difficult to distinguish from other causes of musculoskeletal pain, but diagnostic imaging is easy with methods such as radiography, ultrasound, computer tomography, resonance imaging... On the treatment side, medical therapy is the first-line treatment with nonsteroidal anti-inflammatory painkillers. However, in fact, we found that there are many cases of persistant pain that resistant to NSAIDS drugs, because the calcific deposits are quite large (size up to 1-2 cm) so that the calcification resorption process persists for a long time. Percutaneous aspiration of calcification under ultrasound guidance is a minimally invasive treatment that reduces the progression of the disease due to nearly completely calcific aspiration. This technique is quite easy to implement and can be widely disseminated. We have also performed this technique for some patients diagnosed with calcific tendonitis at Hanoi Medical University Hospital and had achieve good clinical efficacy.
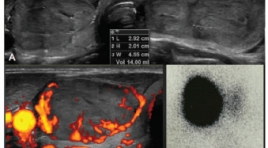
Hiệu quả bước đầu điều trị nhân nóng tuyến giáp bằng phương pháp đốt sóng cao tần
17/03/2020 16:23:44 | 0 binh luận
Initial effectiveness of radiofrequency ablation of the autonomously functioning thyroid nodules SUMMARY Objective: Some patients with autonomously functioning thyroid nodules (AFTN) are not suitable for surgery or radioiodine therapy. Therefore, minimally invasive alternative treatments, such as ethanol ablation or radiofrequency ablation (RFA), are necessary. Methods: This study included seven patients (7 toxic and 10 pretoxic patients; male to female ratio = 1:7.5; mean age, 46.47 ± 13 (range, 22–66) years) who were not eligible for surgery or radioiodine therapy. All of the patients showed hot nodule with suppression of normal thyroid gland in 99mTc pertechnetate scintigraphy. RFA was performed using a 18 gauge internally cooled electrode. Nodule volume, thyroid function, scintigraphy, symptom score (visual analogue scale, 0–10cm), cosmetic grading score (4 point scale), and complications were evaluated before treatment and at 1, 3, 6 months follow-up. Results: Mean volume of the index nodule was 13.07 ± 8.44 (range, 2.2–35.5) mL. After RFA, The volume reduction at 1month, 3 months, 6 months follow up was 42.77 % , 63. % và 78.3 % . Initial mean T3, FT4, and TSH were 2.59 ± 1.19nmol/L, 16.3 ± 5.78pmol/L, and 0.101 ± 0.178 mU/mL, respectively. A significant improvement of mean T3, FT4, and TSH were observed after 1month (T3: 2.18 ± 0.753 nmol/L, p = 0.001; FT4: 14.78 ± 2.86 pmol/L, p = 0.026; TSH: 1.464 ± 0.844 mU/mL, p = 0.001), after 6 months (T3: 2.07 ± 0.614 nmol/L, p = 0.012; FT4: 15.12 ± 2.0 pmol/L, p = 0.001; TSH: 1.269 ± 0.398 mU/ mL, p < 0.001). After ablation, 16 patients became a cold or normal scan and one patient uptake similar normal thyroid tissue. After 6 months, the mean symptom was reduced from 3.47 ± 1.9 to 0.12± 3.32 (p = 0.001) and cosmetic grading score was reduced from từ 3.59 ± 1.1 tới 1.41± 0.712 (p = 0.712) (p <0.001). No major complications were encountered. Conclusions: RFA was effective and safe for treating autonomously functioning benign thyroid nodules and it might be recommended for treating hot benign thyroid nodules as the first-line treatment
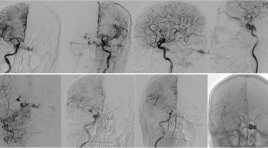
Điều trị can thiệp rò động tĩnh mạch màng cứng xoang hang qua tái thông xoang đá dưới tại Bệnh viện Bạch Mai
04/12/2019 20:27:43 | 0 binh luận
SUMMARY Background: Transvenous coil embolization via inferior petrous sinus (IPS) is a curative and safe method to manage cavernous sinus dural arteriovenous fistulas (CSDAVFs). However, this access will be challenging in case of CSDAVFs associated with angiographic occlusive IPS. Purpose: To report our primary results and experience of transvenous embolization of the CSDAVFs by recanalisation of angiographic occlusive IPS. Methods: Retrospective study of the cases of 12 patients (1 man and 11 women, ranging from 38 years to 79 years of age (mean, 62 years)) who underwent transvenous embolization by recanalisation of angiographic occlusive IPS over a 18 month period. The angioarchitecture of the CSDAVFs, the angiographic as well as the clinical outcomes after embolization and the periprocedural complications were analyzed. Results: True occlusive IPS was found in 12 of the patients. The microcatheter was successfully navigated to the fistula site of the CS in 10 patients (83,3%), while such navigation failed in 2 patients following numerous attempts.The rate of complete occlusion of CSDAVFs was 75%. One case with fatal complication due to MCA occlusion. Conclusion: Angiographic occlusive IPS of CSDAVF may be related to true occlusion of IPS. Transvenous embolization via recanalisation of angiographic occlusive IPS is a safe and effective method to manage CSDAVFs.
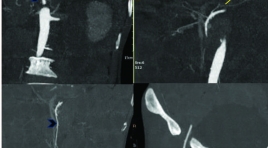
Báo cáo lâm sàng: can thiệp nội mạch cấp cứu điều trị võ giả phình động mạch lách có tình trạng sốc mất máu - một biến chứng ở bệnh nhân viêm tụy cấp
17/03/2020 11:30:29 | 0 binh luận
Splenic artery pseudoaneurysm rupture with hemorrhagic shockas complication of acute pancreatitis treated with emergency endovascular interventions: A case report SUMMARY Background : Rupture of splenic artery pseudoaneurysm (SAPs)secondary to pancreatitis is a uncommon complication, but one with a high mortality rate. Patient generally presented with gastrointestinal bleeding’s symptoms ranging from mild anemia to hemorrhagic shock.Contrast-enhanced abdominal computed tomography (CT) plays an important role in diagnosis, but digital subtraction angiography (DSA) is the gold-standard method to determine the correct diagnosis and make treatment planning. Nowadays, SAPs have been managed with many methods. Endovascular intervention remains the first choice asminimal invasion and a waste of the short time,especially for emergency cases. This article describes a case of SAPs rupture complicated by chronic pancreatitis. Patient admidtted with hypovolemic shock andsuccessfully treated using endovascular coil embolization. Case presentation: A 46 years old man with a past medical histoty of pancreatitisattended to Bach Mai hospital due to hemorrhagic shock as result of acute upper gastrointestinal bleeding. He was intubated and received platelet infusion in secondary hospital.Upper gastrointestinal endoscopyshowed bleeding from the major duodenal papilla, but the source of bleeding remained obscured. CTrevealedrupture of splenic artery pseudoaneurysm causing haemosuccuspancreaticus and duodenal bleeding. Patient immediately managed with coil embolizationby Sandwich technique.After procedure, anemia was controlled steady, butsigns of peritonitis began to appear. At that time, CT images discovered multiple abcesses in hypogastric region and alsso suspectednecrosis of the colonic wall. The patient underwentcolectomy and colostomy in left lumbar region. On the 20th day, he was discharged from hospital with no symptoms and normal blood test. Conclusion: Treatment of acute gastrointestinal bleeding from a splenic artery pseudoaneurysm rupture need to access rapidly and manage reasonably. Emergency endovascular interventions should be the first selection to prevent continous bleeding. Keyword: splenic artery aneurysm rupture, hemorrhagic shock, pancreatitis, emergency endovascular interventions.
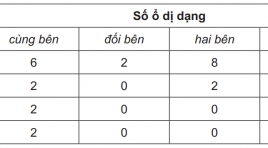
Đánh giá tính an toàn và hiệu quả nút mạch phối hợp bơm trực tiếp ổ dị dạng thông động tĩnh mạch vùng đầu mặt cổ trước phẩu thuật
02/04/2020 22:20:34 | 0 binh luận
Evaluate the safety and effectiveness of ercutaneous direct puncture glue embolization accompanying with endovascular embolization of cervicofacial arteriovenous malformation prior to extirpation SUMMARY: Objects: Evaluate the safety and effectiveness of percutaneous direct puncture glue embolization accompanying with endovascular embolization of cervicofacial arteriovenous malformation prior to extirpation. Subjects and method: Clinical trial without control, achieved in 16 patients in a period from August 2008 to April 2012 at Vietduc Friendship Hospital. Results: 16 patients was carried out endovascular for facial AVM embolization accompanying percutaneous direct puncture embolization, mostly in the age of 20 to 40 (66.5%). There are 20 times of pre-operative embolization, achieving 80% almost occlusion (>80%), extirpation in 94% of cases, hemostatic effect achieved in 88.2%. The length of hospital stay of patients who had one time of embolization and extirpation is 11,9 days. Conclusion: Percutaneous direct puncture accompanying with endovascular glue embolization is a safe and effective procedure, which reduces surgical bleeding and achieves the ability of total extirpation, avoids recurrence. Keyword: arterovenous malformation, endovascular embolization, percutaneous direct puncture, glue.
Bạn Đọc Quan tâm
Sự kiện sắp diễn ra
Thông tin đào tạo
- Những cạm bẫy trong CĐHA vú và vai trò của trí tuệ nhân tạo
- Hội thảo trực tuyến "Cắt lớp vi tính đếm Photon: từ lý thuyết tới thực tiễn lâm sàng”
- CHƯƠNG TRÌNH ĐÀO TẠO LIÊN TỤC VỀ HÌNH ẢNH HỌC THẦN KINH: BÀI 3: U não trong trục
- Danh sách học viên đạt chứng chỉ CME khóa học "Cập nhật RSNA 2021: Công nghệ mới trong Kỷ nguyên mới"
- Danh sách học viên đạt chứng chỉ CME khóa học "Đánh giá chức năng thất phải trên siêu âm đánh dấu mô cơ tim"